Is a probiotic better if it has a higher CFU?
Probiotics are defined as “Live microorganisms which when administered in adequate amounts confer a health benefit to the host”1
However, the specific amount needed to confer a health benefit is not mentioned. This is because the effective dose of probiotics is influenced by a multitude of variables, including health endpoint, the specific probiotic used, delivery vehicle and route of administration2. These factors make it difficult to generalize one optimal dose for probiotic effects.
Therefore, each optimal dose varies between probiotics, their composition, therapeutic effects and administration mode.
Colony-forming units (CFU), is a term used in microbiology to estimate the number of viable (or alive) bacteria found in a sample.
Currently, there is a growing tendency to overdose probiotic products, with doses allegedly ranging from 1 billion to 50 billion CFU several days per week. The number of billions, or even trillions of CFU found in a specific product is frequently used as a promotional asset.
Some products have been shown to be effective at lower levels, while some require substantially more, depending on their probiotic properties.
For instance, clinical trials with specific strains have shown a saturation effect, without differences between high and low dose groups in terms of efficacy3. For this reason, although there is no evidence that higher dosages are unsafe, overdosing is more expensive and unnecessary.
To know if a specific probiotic will have the effects claimed on the package, instead of focusing on CFU, try looking for the following (as states the World Health Organisation)4:
- Bacteria strain codes specified in the pack
- Clinically-proven
- Studied mechanism of action
- No antibiotic resistances
A higher CFU does not necessarily link to a better, more effective probiotic.
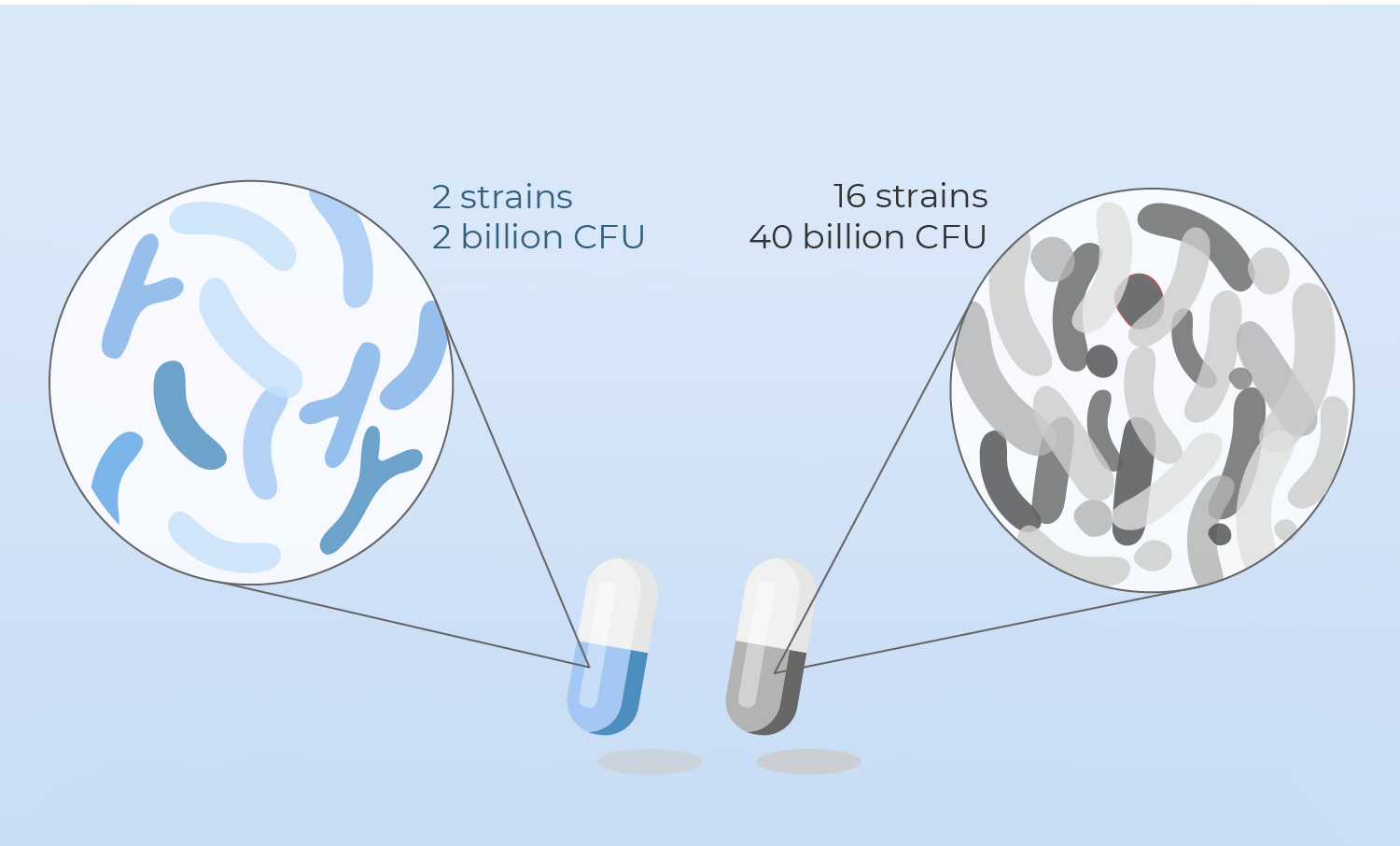
Is a probiotic better if it contains lots of different strains?
Multi-strain probiotics are quite common products found in the health supplements market, gaining popularity every day.
Some claim that, the more strains found in a probiotic, the broader is its efficacy, thanks to the possible synergies among strains. The reality is that no convincing evidence has been found to support these assumptions, as shown in a recent study5.
Although it is true that certain mixtures of probiotics are more effective than their component strains, this observation cannot be generalized.
Choose single-strain, clinically-proven probiotics over multi-strain probiotics without science-based claims.
A higher amount of probiotic strains does not necessarily mean a better, of broader use product.
The effectiveness of the product is not determined additively by the number of strains added, but by the synergistic mixture of key strains. Most importantly, the effectiveness and benefits of the mixture need to be tested in a validated clinical trial6. Two key biological factors help explain this behavior:
- Some strains of probiotics have been documented to produce antimicrobial substances, varying from organic acids to bacteriocins7. Bacteriocins are known for being especially active against close species, g. among different strains of Lactobacilli. Thus, a greater number of strains contained in a probiotic formulation will increase the likelihood of inhibition between them, decreasing their health benefits.
- The more strains are added, the more likely they are to compete for the same nutrients of attachment sites in the gut mucosa. Let’s make it as a comparison: if you imagine the intestine as a surface plenty of flowerpots and the probiotics as seeds to be sown in each of them, if you mix your good, effective seeds with a huge load of other seeds it is clear that less of the good ones will be able to grow in the pots.
Moreover, this issue becomes even more pressing when some strains are added merely to increase the CFU count and have no documented benefit for the host.
References
1. Hill C, Guarner F, Reid G, Gibson GR, Merenstein DJ, Pot B, et al. Expert consensus document. The International Scientific Association for Probiotics and Prebiotics consensus statement on the scope and appropriate use of the term probiotic. Nat Rev Gastroenterol Hepatol. 2014 Aug;11(8):506–14. 2. Guarner F, Sanders MA ER et al. World Gastroenterology Organisation Global Guidelines. Probiotics and prebiotics. 2017. 3. Lorenzo-Zuniga V, Llop E, Suarez C, Alvarez B, Abreu L, Espadaler J, et al. I.31, a new combination of probiotics, improves irritable bowel syndrome-related quality of life. World J Gastroenterol. 2014 Jul;20(26):8709–16. 4. FAO-WHO, Guideline for the Evaluation of Probiotics in Food 2002. 5. Ouwehand AC, Invernici MM, Furlaneto FAC, Messora MR. Effectiveness of Multistrain Versus Single-strain Probiotics: Current Status and Recommendations for the Future. J Clin Gastroenterol. 2018;52 Suppl 1, Proceedings from the 9th Probiotics, Prebiotics and New Foods, Nutraceuticals and Botanicals for Nutrition & Human and Microbiota Health Meeting, held in Rome, Italy from September 10 to 12, 2017:S35–40. 6. Chapman CMC, Gibson GR, Rowland I. Health benefits of probiotics: are mixtures more effective than single strains? Eur J Nutr. 2011 Feb;50(1):1–17. 7. Gillor O, Etzion A, Riley MA. The dual role of bacteriocins as anti- and probiotics. Appl Microbiol Biotechnol. 2008/10/14. 2008 Dec;81(4):591–606.